Bladder Cancer
Bladder Cancer is a commonly diagnosed cancer that typically requires long-term care and disease management. Our experts here at Kentucky Lake Urologic Associates are experts in diagnosing, treating, and managing bladder cancer.
Bladder Cancer Statistics United States
- More than 700,000 men and women have bladder cancer(1)
- Third most common cancer for men(2)
- Incidence is four times higher in men than women(3)
- Incidence is almost 2 times higher in Caucasian men than in African American men(3)
Inside the Bladder
- Bladder cancer occurs in one or more of the four layers of the bladder lining.(4)
- The deeper the layer, the more difficult the cancer is to treat.(4)
- About half the time, it is limited to the uppermost layers (categorized as non-muscle-invasive).(5)
- Approximately a third of cases spread into the third layer, which is muscle (muscle-invasive).(5)
- In most of the remaining cases, the cancer has spread to nearby tissue or lymph nodes outside the bladder.(5)
- In about 4% of cases, it has spread to distant body parts.(5)
Beyond the Bladder(6)
- Bladder cancer can spread beyond the bladder.
- In men, the prostate and seminal vesicles are at risk.
- For women, the risk is to their cervix, uterus, and vagina.
- Can go beyond the pelvic area to lymph nodes around the heart.
- Other organs most commonly at risk are the lung, liver, and bones.
Common Risk Factors(7)
- Smoking: Smokers have double the chances of getting bladder cancer than those who don’t smoke.
- Chemical exposure: Some have been directly linked to bladder cancer, while others are merely suspected.
- Race: Caucasians are at greater risk than African Americans; and Asians have the lowest incidence.
- Age: Risk increases with age, but bladder cancer can occur at any age.
- Gender: Men are at greater risk than women.
- Chronic bladder inflammation: While urinary tract infections, kidney stones and bladder stones don’t cause bladder cancer, they have been linked to it.
Common Signs(s)
- Blood in the urine – even if painless, light, infrequent, or invisible to the naked eye
- Urination irregularities – irritation, urgency, frequency, and/or a constant need to urinate
- A simple urine test or culture can determine whether the signs are serious or not
Means of Diagnosis
- A urine cytology, where a doctor uses a microscope to look for cancer cells in the urine
- An internal bladder exam called a cystoscopy
- A biopsy on suspicious tissue or tumors removed from the bladder
The Cystoscopy(8)
- The gold standard in evaluating the bladder and urethra, as well as diagnosing and monitoring bladder cancer
- Conducted using a long, thin camera (a cystoscope) inserted through the urethra into the bladder
- Done in an operating room under general anesthesia or in a medical office with moderate sedation or pain management
- A standard cystoscopy uses everyday white light to help the doctor visually assess the general health of the bladder and find irregularities to be further investigated
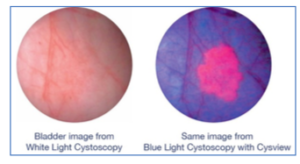
Blue Light Cystoscopy with Cysview® (hexaminolevulinate HCl)(9)
- Here at HCMC’s Kentucky Lake Urologic Associates our urologists have the option to enhance a cystoscopy procedure with the latest technology – blue light equipment and an optical imaging agent called Cysview.
- Cysview makes bladder cancer glow bright pink under blue light.
- The addition of blue light and Cysview can significantly improve detection of non-muscle-invasive bladder cancer compared to white light alone.
- With enhanced visibility, more cancer can be removed.
Staging and Grading(10)
Staging identifies location of a bladder cancer tumor in relation to the bladder’s inner lining. Knowing the stage helps the doctor can plan the best treatment.
- Is the cancer limited to the bladder lining?
- Has the cancer invaded the bladder wall?
- Has the cancer spread beyond the bladder?
- Where else has the cancer spread?
These are the different stages of bladder cancer:
- T0: No tumor
- Ta: Papillary tumor that has not invaded the bladder wall
- TIS (CIS): Carcinoma in situ, which is a non-invasive, flat, high-grade (G3) cancer
- T1: Tumor that has invaded the connective tissue under the surface lining of the bladder
- T2: Tumor has invaded the muscle layer
- T3: Tumor has penetrated the bladder wall and invaded the fat layer
- T4: Tumor has invaded other organs
References: 1. National Cancer Institute. SEER Stat Facts: Bladder Cancer 2017. https://seer.cancer.gov/statfacts/html/urinb.html. Accessed January 25, 2019.
2. Globocan. Prevalence by population 2018. Available at: http://gco.iarc.fr/today/online-analysis- table?v=2018&mode=cancer&mode_population=continents&population=900&populations=840&key=asr&sex=0&cancer=39&type=2&statistic=5&prevalence=1&population _group=0&ages_group%5B%5D=0&ages_group%5B%5D=17&nb_items=5&group_cancer=1&include_nmsc=1&include_nmsc_other=1#collapse-group-0-2. Accessed February 26, 2020. 3. American Cancer Society. Cancer Facts and Figures 2017. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and- statistics/annual-cancer-facts-and-figures/2017/cancer-facts-and-figures-2017.pdf. Accessed July 15, 2019. 4. Bladder Cancer Advocacy Network. What is Bladder Cancer? https://www.bcan.org/what-is-bladder-cancer/. Accessed July 15, 2019. 5. American Cancer Society. Key Statistics for Bladder Cancer 2019. https://www.cancer.org/cancer/bladder-cancer/about/key-statistics.html. Accessed March 25, 2019. 6. Baylor College of Medicine. Bladder Cancer. https://www.bcm.edu/healthcare/care-centers/urology/conditions/bladder-cancer. Accessed July 15, 2019. 7. Bladder Cancer Advocacy Network. Bladder Cancer Symptoms, Signs and Risk Factors. https://www.bcan.org/signs-symptoms/. Accessed July 15, 2019. 8. Bladder Cancer Advocacy Network. Diagnosing and Monitoring Bladder Cancer. https://www.bcan.org/diagnosing-and-monitoring/. Accessed July 15, 2019. 9. Cysview [prescribing information]. 2018:1-14. 10. Bladder Cancer Advocacy Network. Diagnosing and Monitoring Bladder Cancer. https://www.bcan.org/types-stages-grades/. Accessed July 15, 2019.
Cysview (hexaminolevulinate HCl) Indication
Cysview is an FDA-approved optical imaging agent indicated for use in the cystoscopic detection of non-muscle invasive bladder cancer including carcinoma in situ (CIS) among patients suspected or known to have lesion(s) on the basis of a prior cystoscopy. Cysview is used with the KARL STORZ Photodynamic Diagnostic (PDD) system to perform BLC as an adjunct to White Light Cystoscopy.











